We have all likely seen eosinophils vanish from the blood after starting steroids. What is going on? This was the topic of Episode 32 of the podcast.
By way of background, eosinophils (named for their red color with hematoxylin and eosin staining) are granulocytic white blood cells that develop in the bone marrow and reside primarily in tissues. They have numerous physiologic functions, from defense against parasites to immune regulation. They also play a primary role in the pathogenesis of certain types of asthma.
Yes, that Fauci
One of the earliest groups to examine the connect between steroids and eosinopenia was Anthony Fauci looked. In the 1970s they found that within 4 hours of steroid exposure, there was a marked decline in eosinophil counts in the blood.

There are at least three different explanations for this:
- Decreased production of eosinophils from the bone marrow
- Redistribution of existing eosinophils from the blood into tissues (where they can’t be measured)
- Destruction of eosinophils in the periphery
We’ll look at each of these three mechanisms.
Decreased Production
There is evidence of decreased eosinophils production after exposure to corticosteroids, at least in vitro. This was first noted in a 1985 study in the Journal of Clinical Investigation. The investigators studied how steroid exposure affected proliferation of different white blood cells, specifically eosinophils, neutrophils, and macrophages. They specifically extracted bone marrow progenitors for each cell type and exposed them to hydrocortisone. The hydrocortisone reduced new eosinophil development, but had no effect on neutrophils or macrophages.
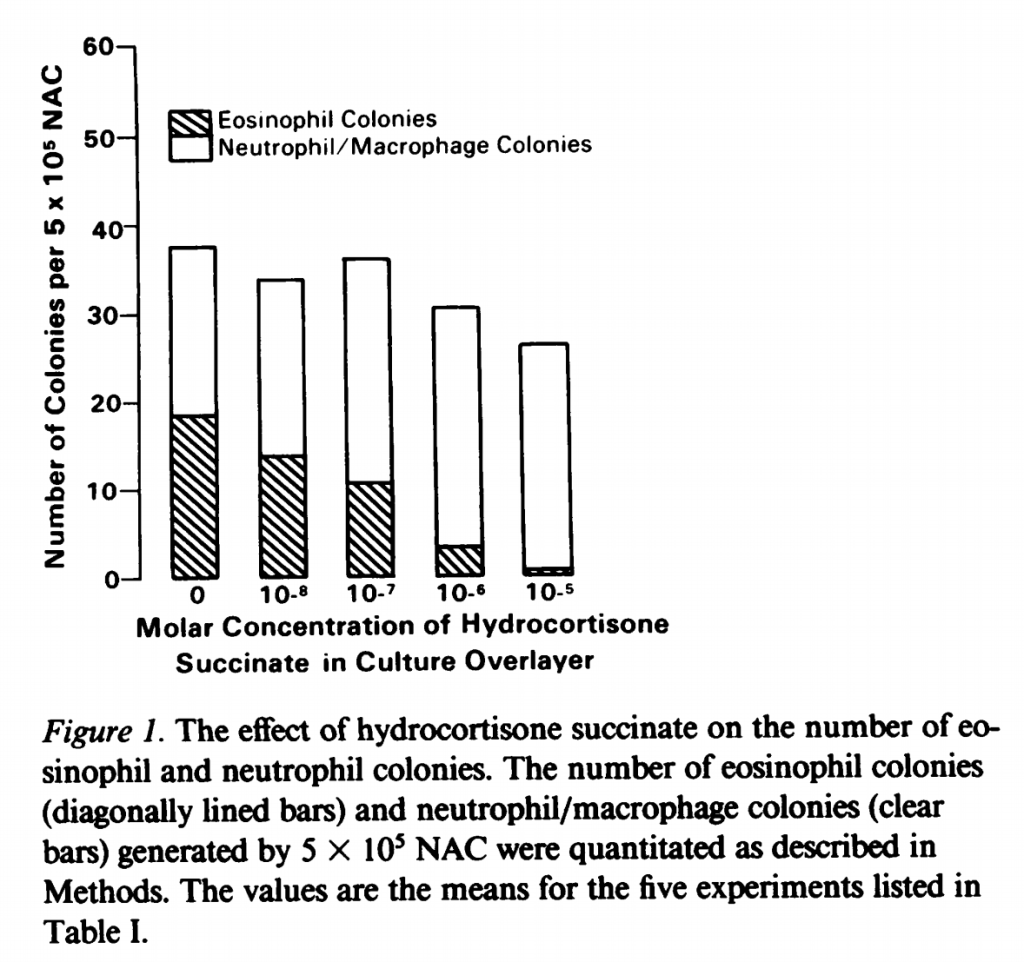
The mechanism may relate to decreased synthesis of cytokines that stimulate eosinophil growth and development, specifically IL-5 and GM-CSF, as well as their cellular effects. But this cannot be the whole story. Why?
Eosinophils have a half-life in the blood stream of 18 hours. This is far longer than the time it takes for eosinophil counts to drop after exposure to steroids, which Fauci’s study suggested occurred as early as 4 hours.
Redistribution
When discussing redistribution we are specifically talking movement to compartments other than the bloodstream. It is important to remember that the vast majority of eosinophils normally reside in tissues and not the blood. So redistribution out of the blood would sort of be an accentuation of a normal equilibrium.
Animal studies suggest that eosinophil redistribution does occur after steroid exposure. In one experiment in rats, giving them cortisol caused eosinophils to migrate out of the blood and into lymphoid tissues, such as the spleen and lymph nodes. In the same experiment, splenectomy prior to cortisol exposure actually preserved blood eosinophil counts, compared to rats w/ intact spleens. Removing the spleen took away the site of redistribution.
Regarding the mechanism, there is some recent literature in Rhesus Macaques suggesting that CXCR4 (a chemokine receptor) is responsible for eosinophil homing to the bone marrow after prednisone. It’s not clear that CXCR4 plays a similar role in chemotaxis to the spleen and other lymphoid organs.
So, it’s destruction, isn’t it?
Destruction
Recall that steroids block the release of cytokines that support eosinophil development in the bone marrow, specifically IL-5 and GM-CSF. These cytokines also promote eosinophil survival, potentially by inhibiting apoptosis. You would expect that since steroids inhibit IL-5 and GM-CSF, they should shorten eosinophil lifespan. And accelerated cell death is exactly what happens when eosinophils are exposed to steroids.
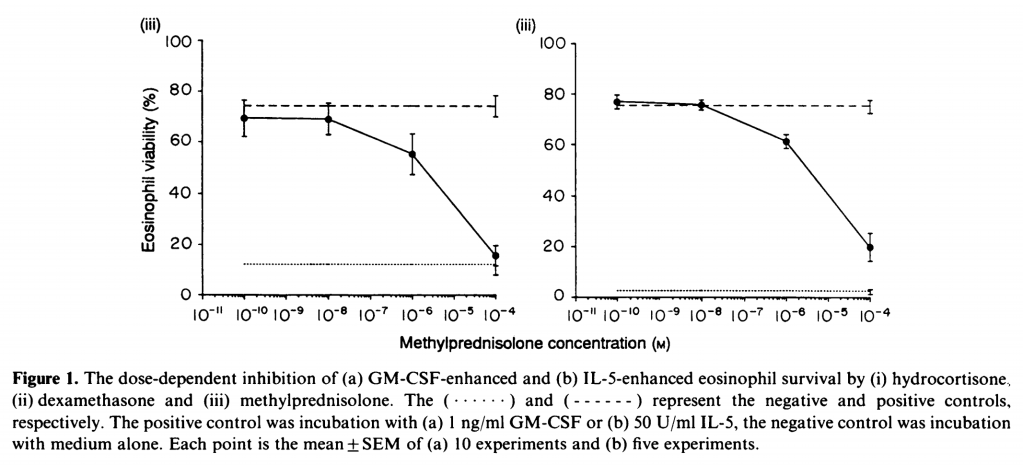
Is the inverse true?
The mechanism of peripheral eosinophilia that can accompany adrenal insufficiency likely relates to the inverse of the above. Adrenal insufficiency is associated with eosinophilia because it is a state of deficiency of endogenous corticosteroids.
Another clinical correlate is around the group of disease known as the hypereosinophilic syndromes, which are defined as blood eosinophilia ≥1500/mm3 and eosinophil-related clinical manifestations. The cornerstone of initial therapy for these disorders generally involves corticosteroids for most of these disorders, up to 15% of patients are steroid non-responders. That is, their blood eosinophil counts do not meaningfully decrease with steroid exposure. Preliminary in vitro data suggests that over-expression of IL-5 may contribute to this phenomenon.
Take Home Points
- Blood eosinophil counts drop within 4 hours of exposure to steroids, probably for 3 different reasons: decreased production, redistribution, and destruction.
- Steroids inhibit the cytokines GM-CSF and IL-5 release and cellular effects, which contributes to decreased eosinophil production and accelerated cell death.
- Redistribution to lymphoid organs may relate to steroids effects on CXCR4.
- The peripheral eosinophilia of adrenal insufficiency relates to the reduced production of endogenous corticosteroids.
CME/MOC
Click here to obtain AMA PRA Category 1 Credits™ (1.00 hours), Non-Physician Attendance (1.00 hours), or ABIM MOC Part 2 (1.00 hours).
Listen to the episode
https://oembed.libsyn.com/embed?item_id=20178899
Credits & Citation
◾️Episode written by Avi Cooper
◾️Show notes written by Tony Breu and Avi Cooper
◾️Audio edited by Clair Morgan of nodderly.com
Cooper AZ, Abrams HR, Breu AC. Why do eosinophils vanish from the blood after treatment with corticosteroids? The Curious Clinicians Podcast. August 18, 2021
Image credit: https://www.verywellhealth.com/guide-to-eosinophils-797211
Related tweetorial: https://x.com/AvrahamCooperMD/status/1304825763984703489

