For this episode of the podcast, we discuss something Hannah became interested in after seeing a question about it on Twitter. Here’s a link to Hannah’s explanation on the topic and the original case tweet.
GFR basics
To understand why TMP/SMX might lead to an increase in creatinine without a fall in renal function, we need to first understand a few features of glomerular filtration rate (GFR) measurement. When we measure GFR, we aim to determine the amount of filtrate moving past all the combined glomeruli without evaluating what’s going on in the downstream renal tubules.
If we’re evaluating GFR using a blood (i.e., serum) test, the ideal molecular we measure would reflect changes in GFR and only changes in GFR. With this in mind, it’s worth listing all the changes that might lead to an increase in the serum value for any molecular handled by the kidney. In theory, there are 5 causes:
- Increased production
- Decreased glomerular filtration
- Increased metabolism in the kidney
- Decreased tubular reabsorption
- Increased tubular excretion
To be an ideal marker of GFR, a molecular would be freely filtered and we would only see an increase in the serum value when glomerular filtration decreased. We actually have that perfect marker: inulin (a fructose polymer). We don’t use it as our measure of GFR because it is a pain to measure (it has to be injected and requires an assay not available in most laboratories).
What’s the problem with creatinine?
Creatinine remains our go-to for measuring GFR. But remember, an optimal marker of GFR would only see a change in the plasma level based on a change in filtration. When we see a rise in creatinine, we typically assume this reflects a decrease in glomerular filtration rate. We’re usually right.
But every once in a while we have to think about the other ways molecules’ serum value might increase. That’s because although creatinine is produced at a (mostly) stable and predictable rate by our muscle tissue, rhabdomyolysis might theoretically lead to an increase in creatinine from damage itself (this is not certain). And although it is freely filtered and does not undergo reabsorption or metabolism by the kidney, it DOES undergo secretion in the proximal tubule. Normally, increased production and increased secretion of creatinine aren’t clinically relevant. But, occasionally, they are. Enter TMP/SMX.
How does TMP/SMX increase creatinine?
There are a number of transporters that move creatinine from the blood into the cells of the tubule and then out the luminal side into the urine; these include:
◾️organic anion transporter 2 (OAT2)
◾️multidrug and toxin extrusion protein 1 and 2K (MATE1 and MATE2K)
◾️organic cation transporter 2 (OCT2)
Trimethoprim (TMP) is a weak organic base, and has a slightly positive charge at physiologic pH. It is secreted in the renal tubules through many of the same transporters used by creatinine: specifically OCT2 and MATE1. So, when a patient has a high dose of TMP in their system, it competes with creatinine for the transporters. When less creatinine is being into the urine more of it stays in the blood. Result: an increase in serum creatinine despite a stable GFR!
What % rise in Cr might be attributable to TMP/SMX?
The short answer: in one study of healthy subjects, 200 mg BID (a double-strength tab contains 160 mg) induced a rise of about 20-25%. There are other factors that might affect creatinine secretion with concomitant TMP (e.g., individual patient polymorphisms in relevant genes, dose of the drug, and all the other factors that might affect creatinine).
Also, it is important to remember that a rise in creatinine in patients receiving TMP/SMX may actually reflect acute kidney injury. One study from the Michael E. Debakey VA Medical Center in Houston looked at inpatients who had gotten TMP/SMX and remained inpatient long enough to get follow-up labs. In their sample of 500 patients, 6% had a rise in both BUN and creatinine, suggesting a true drop in GFR.
How else might TMP/SMX increase creatinine?
There are at least four mechanism by which TMP/SMX might cause acute kidney injury:
- Acute interstitial nephritis (AIN): As a sulfa drug, TMP/SMX can cause AIN, although there was only 1 case documented in the VA cohort. No patients had eosinophils in their urine.1
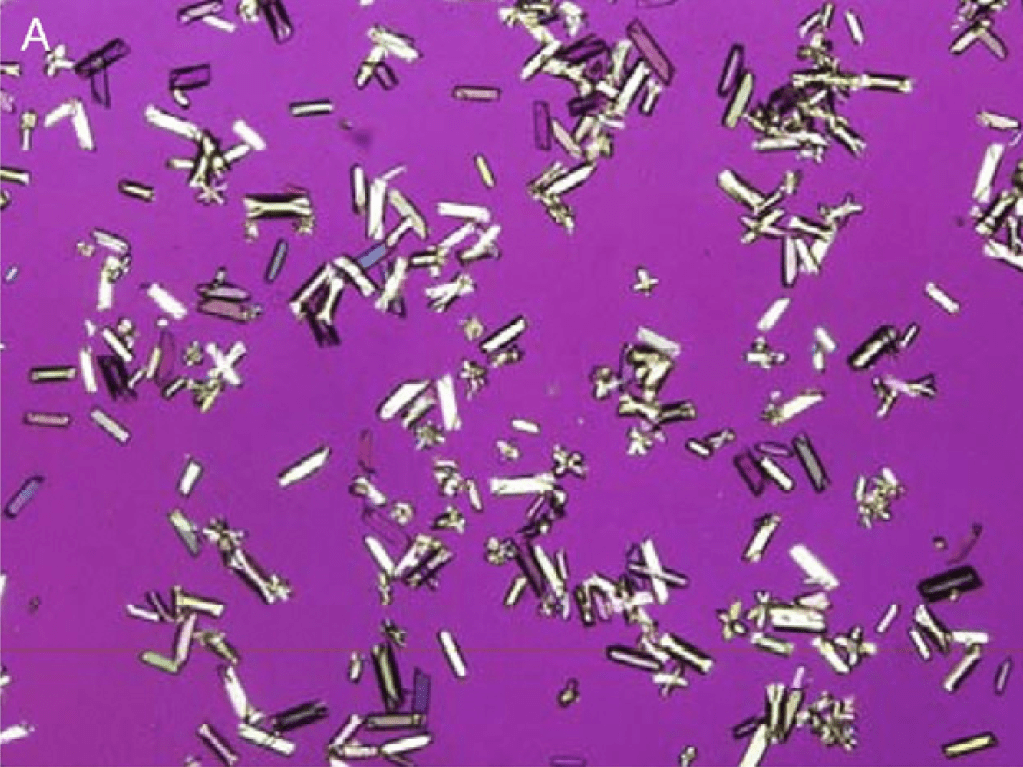
- Crystal formation: In volume depleted patients who have gotten TMP/SMX, crystals can precipitate and form (see Picture of birefringent pleomorphic crystalluria on polarized microscopy from Shrishrimal and Wesson). As an interesting pearl, patients who are hypoalbuminemic or have other drugs on board that might bind albumin (e.g., penicillin) the concentration of free TMP/SMX can be high enough to cause it to precipitate even if the patient isn’t volume depleted.
- Increasing the concentration of other nephrotoxic drugs: Recall that TMP competes with creatinine for secretion via that multidrug and toxin excretion protein. Unsurprisingly, multiple drugs and toxins are also excreted by that protein. Examples include cimetidine, pyramethamine, dolutegravir, and metformin. One study found that receiving metformin and TMP saw an increase in the maximum plasma concentration of metformin by 37%! While metformin does not directly cause AKI, other nephrotoxic drugs including chemotherapeutic agents can have their levels similarly increased by TMP. It is also worth noting that TMP/SMX also inhibits CYP P450 2C8/9, which can lead to supratherapeutic warfarin and sulfonylurea levels.
- Acute tubular necrosis (ATN) has also been noted as a rare side effect of TMP/SMX.
TMP-associated hyperkalemia
Trimethoprim also acts like the K-sparing diuretic amiloride at the epithelial sodium channels (ENaC) of the collecting duct. People who are already hyporeninemic and who have hypoaldosteronism (e.g., those on ACE inhibitors or with chronic diabetic nephropathy) are at higher risk of hyperkalemia with the use of TMP/SMX. This is also more common with higher doses.
Take home points
- In additional to being filtered by the glomerulus, creatinine is also secreted in the proximal tubule.
- The trimethoprim component of TMP/SMX is secreted using the same transporters. As a result, TMP competes with creatinine, leading to decreased tubule secretion and increased serum blood. This doesn’t necessarily reflect a fall in GFR.
- If you prescribe TMP/SMX and do see an increase in creatinine, look at the BUN and urine output for other clues about renal function.
- Given that other medications compete with creatinine and TMP for the renal transports, perform a medication reconciliation after seeing an increase in creatinine in patients receiving TMP/SMX.
- TMP/SMX can also cause an acute rise in potassium.
Learning Objectives
- Review the physiology behind measurement of glomerular filtration rate.
- Explain why trimethoprim/sulfamethoxazole might lead to an isolated increase in creatinine.
- Develop an approach to a rise in creatinine associated with trimethoprim/sulfamethoxazole, including potential causes of acute kidney injury.
- Illustrate the pathophysiology of hyperkalemia associated with trimethoprim use.
CME/MOC
We are excited that The Curious Clinicians have partnered with VCU Health Continuing Education to offer continuing education credits for physicians and other healthcare professionals. Visit VCU Health for more information.
Listen to the episode
Credits & Citation
◾️Episode written and edited by Hannah Abram
◾️Show notes by Tony Breu and Hannah Abrams
Abrams HR, Cooper AZ, Breu AC. Why does TMP/SMX cause an isolated rise in creatinine? The Curious Clinicians Podcast. June 24, 2020. https://curiousclinicians.com/2020/06/24/episode-3-why-does-tmp-smx-cause-an-isolated-rise-in-creatinine/
Opening image source (E. coli dividing): https://phil.cdc.gov//PHIL_Images/10042/10042.tif
1It should be noted that checking urine eosinophils is a Thing We Do For No ReasonTM given their low sensitivity.